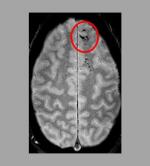
A new study indicates that traumatic microbleeds
could be potential biomarkers for determining
treatments for traumatic brain injuries
could be potential biomarkers for determining
treatments for traumatic brain injuries
US researchers find new insights on the importance of traumatic microbleeds
October 18, 2019
by John R. Fischer, Senior Reporter
Research into traumatic brain injury has uncovered new insights about traumatic microbleeds that may change perceptions on the development of treatments and drugs.
U.S. scientists have found that damage to blood vessels following head injury may help predict future health problems and disabilities, and could be a potential biomarker for determining which patients would benefit from treatments that target vascular injury.
"Traumatic microbleeds may represent injury to blood vessels that occur following even minor head injury," said Lawrence Latour, a researcher at the National Institute of Neurological Disorders and Stroke (NINDS), part of the National Institutes of Health, and senior author of the study, in a statement. "While we know that damage to brain cells can be devastating, the exact impact of this vascular injury following head trauma is uncertain and requires further study."
The study utilized MR rather than CT, due to microbleeds typically being too small to detect with the latter modality.
One part, performed by Cold Spring Harbor Laboratory, involved a postmortem scan of an injured brain. Utilizing a high-throughput neurohistological pipeline consisting of various techniques for labeling and visualizing brain slices, the lab team digitally analyzed the postmortem tissue at micron resolution and correlated the findings with those of MR scans for a clearer view of vascular injury incurred.
The researchers at CSHL found greater blood vessel damage than that of nerves, with an iron stain revealing a significant amount of blood cells across the area of the brain where surrounding lesions were located. A myelin stain used to show nerve fiber fragments did not show any significant damage.
This, according to the team, is a sign of traumatic microbleeds caused by ruptures along blood vessels across the brain, and with more research, could affect treatment development for TBI, which is mainly influenced by the long-standing hypothesis that that blunt force from TBI causes nerve damage.
"Nerve damage following traumatic brain injuries has been a majority point of view, and therapy as well as drug development has been targeted toward that," said Cold Spring Harbor Laboratory professor Partha Mitra in a statement. "The idea is that if the mechanism is actually different, therapeutic intervention may also be different."
Another part, headed by NINDS, examined 439 adults treated in the emergency department for head injuries, who received MR scans within 48 hours of their injury and again during four follow-up visits. They also completed behavioral and outcome questionnaires.
Of all participants, 31 percent showed signs of microbleeds. Fifty-eight percent of those with severe head injury showed indications, as did 27 percent of mild cases. Microbleeds appeared as either linear streaks or dotted lesions, and those who showed signs of them had both types. Frontal lobes were the part of the brain most likely to incur microbleeds, and those with them were more likely to experience a greater level of disability compared to those who did not have them.
The authors were unable to determine the direction of the relationship between TMBs and acute injuries, but specify that future research may reveal how much information about head injuries can be extracted from the presence of microbleeds, and to help clinicians determine which patients should undergo specific imaging following head injuries.
"Combining these technologies and methods allowed us to get a much more detailed look at microbleed structure and get a better sense of just how extensive they are," said Allison Griffin, a graduate student and first author of the paper, in a statement.
Disability in patients was determined by a commonly used outcome scale. No evidence from the study suggests that MR scans should replace CT for suspected head injury.
Other participants included the University of Maryland and the Center for Neuroscience and Regenerative Medicine at the Uniformed Services University of the Health Sciences.
The findings are supported by the NIH Intramural Research Program.
U.S. scientists have found that damage to blood vessels following head injury may help predict future health problems and disabilities, and could be a potential biomarker for determining which patients would benefit from treatments that target vascular injury.
"Traumatic microbleeds may represent injury to blood vessels that occur following even minor head injury," said Lawrence Latour, a researcher at the National Institute of Neurological Disorders and Stroke (NINDS), part of the National Institutes of Health, and senior author of the study, in a statement. "While we know that damage to brain cells can be devastating, the exact impact of this vascular injury following head trauma is uncertain and requires further study."
The study utilized MR rather than CT, due to microbleeds typically being too small to detect with the latter modality.
One part, performed by Cold Spring Harbor Laboratory, involved a postmortem scan of an injured brain. Utilizing a high-throughput neurohistological pipeline consisting of various techniques for labeling and visualizing brain slices, the lab team digitally analyzed the postmortem tissue at micron resolution and correlated the findings with those of MR scans for a clearer view of vascular injury incurred.
The researchers at CSHL found greater blood vessel damage than that of nerves, with an iron stain revealing a significant amount of blood cells across the area of the brain where surrounding lesions were located. A myelin stain used to show nerve fiber fragments did not show any significant damage.
This, according to the team, is a sign of traumatic microbleeds caused by ruptures along blood vessels across the brain, and with more research, could affect treatment development for TBI, which is mainly influenced by the long-standing hypothesis that that blunt force from TBI causes nerve damage.
"Nerve damage following traumatic brain injuries has been a majority point of view, and therapy as well as drug development has been targeted toward that," said Cold Spring Harbor Laboratory professor Partha Mitra in a statement. "The idea is that if the mechanism is actually different, therapeutic intervention may also be different."
Another part, headed by NINDS, examined 439 adults treated in the emergency department for head injuries, who received MR scans within 48 hours of their injury and again during four follow-up visits. They also completed behavioral and outcome questionnaires.
Of all participants, 31 percent showed signs of microbleeds. Fifty-eight percent of those with severe head injury showed indications, as did 27 percent of mild cases. Microbleeds appeared as either linear streaks or dotted lesions, and those who showed signs of them had both types. Frontal lobes were the part of the brain most likely to incur microbleeds, and those with them were more likely to experience a greater level of disability compared to those who did not have them.
The authors were unable to determine the direction of the relationship between TMBs and acute injuries, but specify that future research may reveal how much information about head injuries can be extracted from the presence of microbleeds, and to help clinicians determine which patients should undergo specific imaging following head injuries.
"Combining these technologies and methods allowed us to get a much more detailed look at microbleed structure and get a better sense of just how extensive they are," said Allison Griffin, a graduate student and first author of the paper, in a statement.
Disability in patients was determined by a commonly used outcome scale. No evidence from the study suggests that MR scans should replace CT for suspected head injury.
Other participants included the University of Maryland and the Center for Neuroscience and Regenerative Medicine at the Uniformed Services University of the Health Sciences.
The findings are supported by the NIH Intramural Research Program.