Imaging heart disease in the era of COVID-19
April 05, 2021
by Lauren Dubinsky, Senior Reporter
A growing body of research is revealing that the connection between COVID-19 and heart problems is significant.
“As the pandemic progressed, so has understanding of the impact the virus can have on a patient’s heart,” Dagfinn Saetre, general manager of cardiovascular ultrasound at GE Healthcare told HCB News. “Doctors and researchers have observed a particular connection between COVID-19 and strain on the heart’s right ventricle.”
A study conducted last year by Mount Sinai Heart found that hospitalized COVID-19 patients with right ventricular dilation might be at a higher risk of poor outcomes and even death. Another recent study published in JAMA Cardiology found that heart problems were the cause of death among 50% of the 416 COVID-19 patients in Wuhan, China.
In response, the American Society of Echocardiography (ASE) and the European Association of Cardiovascular Imaging (EACVI) recommended that clinicians perform limited echo exams on COVID-19 patients at the point-of-care to monitor their left and right ventricles for cardiac dysfunction.
Saetre reported that clinicians have been relying on GE’s Vivid ultrasound systems to assess the left and right ventricle throughout the pandemic. In October, the company received FDA approval for its Vivid Ultra Edition system, which features AI-driven algorithms for 2D and doppler echo imaging.
DiA Imaging Analysis has also seen an increase in the use of its products, especially its cardiac artificial intelligence (AI) tools. This uptick is the result of point-of-care settings triaging and monitoring COVID-19 patients’ hearts.
The downside of point-of-care ultrasound
Point-of-care ultrasound (POCUS) is number two on ECRI Institute’s 2020 list of Top 10 Health Technology Hazards. That’s because these systems are not being used appropriately leading to misdiagnoses, and there is an overreliance on this modality when a more comprehensive exam by an imaging specialist is needed.
Additionally, there is a lack of universal guidelines or recommendations for POCUS and training for this modality is inconsistent. ECRI recommends that healthcare facilities create a multi-disciplinary POCUS committee to oversee the standardization of this technology within the facility.
DiA launched two FDA-approved and CE-marked AI solutions in 2020 that help make cardiac ultrasound exams easier to perform. The new LVivo RV assesses the size and function of the right ventricle (RV) to check for cardiac dysfunction such as pulmonary embolism and pulmonary hypertension as well as potential heart failure.
“The RV has always been very difficult to evaluate, due to its unique structure and location,” said Hila Goldman-Aslan, CEO and cofounder at DiA. “Additionally, RV analysis using 2D ultrasound is currently done visually or manually, making the process time-consuming, error-prone and highly dependent on the user’s experience.”
“DiA's technology is based on advanced pattern recognition, deep learning and machine learning algorithms that automatically imitate the way the human eye detects image borders and identifies motion,” said Goldman-Aslan.
Philips Healthcare also has a stake in this market with its newly FDA-cleared 3D Auto RV application that leverages AI-based techniques. This product was the fruit of the company’s acquisition of TOMTEC in 2017.
“Until recently, analysis of the right heart was relatively uncommon, but the advent of new, A.I.-based techniques is helping to give greater confidence to sonographers and cardiologists that are seeking to add RV measurements to their analysis in a reproducible and efficient manner,” said Dr. Alexandra Goncalves, head of the medical office for precision diagnostic at Philips.
The rise of GLS
In January 2019, myocardial strain earned a category 1 reimbursement code in the U.S. The use of strain imaging as a prognostic indicator of left ventricular function is now widely recognized as a clinical best practice.
“The global longitudinal strain (GLS) of all the different strain methodologies that we've had has become the one that people use,” said Michael McElroy, solutions marketing senior manager at Canon Medical Systems USA. “We finally have a standard of strain.”
Strain imaging provides an earlier prediction of cardiac issues before the ejection fraction (EF) changes. By the time the EF changes, that’s the indicator of major issues with myocardial function.
Last year, Canon released its Auto EF with GLS tool for its Aplio a-series and i-series ultrasound systems. By hitting one button, this tool automatically provides the clinician with the EF and GLS number.
Finding the right views in each echo exam and EF and GLS is also a cumbersome process. This task typically takes stenographers a couple of minutes to complete, but they can get those numbers in a couple of seconds with this tool.
DiA also launched a new tool for this called LVivo Seamless. It automatically obtains optimal views and cardiac measurements for every cardiac ultrasound exam in the echo lab.
There are usually between 50 and 60 views in a standard echo exam and this tool pre-selects the optimal views for the calculation of EF and GLS.
An area that GLS is showing promise in is chemotherapy. Many chemotherapy agents can damage the heart muscle, so GLS is being used with the highest sensitivity to assess any potential damage.
“The tightrope that the oncologist is walking is whether they can use the agent and not put the patient in unrecoverable heart failure because of the myocardial toxicity of the agent,” said McElroy.
GLS strain imaging provides an earlier indication of chemotherapy toxicity before the EF changes. It’s thought that once the EF goes down, the damage is permanent, but if the clinician spots the change in strain GLS early on, they can adjust the chemotherapy regimen and preserve the EF and have good oncological and cardiological outcomes.
Despite its benefits, adoption remains slow. According to McElroy, the routine use of strain imaging among cardiologists is within the 20 to 30 percent range, its use in doctor’s offices is about 10 percent and at the university level it’s upwards of 100 percent.
Structural heart disease
The global structural heart devices market is projected to reach $13 billion in 2027, according to a new Transparency Market Research report. New procedures for aortic stenosis and mitral regulation are driving this trend, as well as the rising geriatric population.
“Considering the growing number of structural heart procedures, innovations in this area are game changers,” said Elizabeth Oakes, senior director, clinical strategy at Siemens Healthineers.
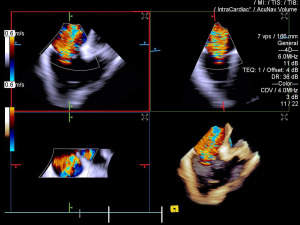
The company recently launched a product that has the potential to greatly improve procedural efficiency in this area. The latest ACUSON SC2000 PRIME 6.0 ultrasound system features 4D Volume Intracardiac Echocardiography (ICE) capability with the ACUSON AcuNav Volume ICE catheter.
This is currently the only commercially available 4D Volume ICE catheter on the market as of February 2021. It provides more real-time information in one view to accurately navigate, guide and measure with multiplanar reconstruction planes (MPRs).
This technology also has the potential to reduce the need for general anesthesia as well as scheduling effort, staffing needs, procedural time, and cost compared to transesophageal echocardiogram (TEE)-guided procedures.
A 2017 study published in JACC: Cardiovascular Interventions found that left atrial appendage closure procedures performed with ICE led to 57 percent time savings per case compared to TEE.
4D Volume ICE allows physicians to offer treatment to patients that would otherwise have no options for structural heart disease procedures. These patients cannot undergo TEE or general anesthesia, or any procedure that requires optimal imaging of the tricuspid valve.
Philips is also making headway in this field with its new automated tools for mitral valve and left atrial appendage measurement, Auto MVA and LAA solution, and its new visualization tools, TrueVue Glass. These tools are for use with the company’s EPIQ CVx ultrasound system.
“[Our new tools] provide a unique way of analyzing the heart structure and function with transparency,” said Philips’ Goncalves.
During interventional echo procedures, the system visualizes the morphology of the left atrial appendage (LAA) and automatically measures the ostium. It also automatically assesses the mitral valve and obtains multiple measurements and functional data.
“2020 was a year of innovation with exciting new features for assessment of structural heart disease and procedure guidance,” said Goncalves. “3D techniques have been evolving to provide better visualization, efficient quantification and safe guidance for the challenging structural heart disease procedures.”
“As the pandemic progressed, so has understanding of the impact the virus can have on a patient’s heart,” Dagfinn Saetre, general manager of cardiovascular ultrasound at GE Healthcare told HCB News. “Doctors and researchers have observed a particular connection between COVID-19 and strain on the heart’s right ventricle.”
A study conducted last year by Mount Sinai Heart found that hospitalized COVID-19 patients with right ventricular dilation might be at a higher risk of poor outcomes and even death. Another recent study published in JAMA Cardiology found that heart problems were the cause of death among 50% of the 416 COVID-19 patients in Wuhan, China.
In response, the American Society of Echocardiography (ASE) and the European Association of Cardiovascular Imaging (EACVI) recommended that clinicians perform limited echo exams on COVID-19 patients at the point-of-care to monitor their left and right ventricles for cardiac dysfunction.
Saetre reported that clinicians have been relying on GE’s Vivid ultrasound systems to assess the left and right ventricle throughout the pandemic. In October, the company received FDA approval for its Vivid Ultra Edition system, which features AI-driven algorithms for 2D and doppler echo imaging.
DiA Imaging Analysis has also seen an increase in the use of its products, especially its cardiac artificial intelligence (AI) tools. This uptick is the result of point-of-care settings triaging and monitoring COVID-19 patients’ hearts.
The downside of point-of-care ultrasound
Point-of-care ultrasound (POCUS) is number two on ECRI Institute’s 2020 list of Top 10 Health Technology Hazards. That’s because these systems are not being used appropriately leading to misdiagnoses, and there is an overreliance on this modality when a more comprehensive exam by an imaging specialist is needed.
Additionally, there is a lack of universal guidelines or recommendations for POCUS and training for this modality is inconsistent. ECRI recommends that healthcare facilities create a multi-disciplinary POCUS committee to oversee the standardization of this technology within the facility.
DiA launched two FDA-approved and CE-marked AI solutions in 2020 that help make cardiac ultrasound exams easier to perform. The new LVivo RV assesses the size and function of the right ventricle (RV) to check for cardiac dysfunction such as pulmonary embolism and pulmonary hypertension as well as potential heart failure.
“The RV has always been very difficult to evaluate, due to its unique structure and location,” said Hila Goldman-Aslan, CEO and cofounder at DiA. “Additionally, RV analysis using 2D ultrasound is currently done visually or manually, making the process time-consuming, error-prone and highly dependent on the user’s experience.”
“DiA's technology is based on advanced pattern recognition, deep learning and machine learning algorithms that automatically imitate the way the human eye detects image borders and identifies motion,” said Goldman-Aslan.
Philips Healthcare also has a stake in this market with its newly FDA-cleared 3D Auto RV application that leverages AI-based techniques. This product was the fruit of the company’s acquisition of TOMTEC in 2017.
“Until recently, analysis of the right heart was relatively uncommon, but the advent of new, A.I.-based techniques is helping to give greater confidence to sonographers and cardiologists that are seeking to add RV measurements to their analysis in a reproducible and efficient manner,” said Dr. Alexandra Goncalves, head of the medical office for precision diagnostic at Philips.
The rise of GLS
In January 2019, myocardial strain earned a category 1 reimbursement code in the U.S. The use of strain imaging as a prognostic indicator of left ventricular function is now widely recognized as a clinical best practice.
“The global longitudinal strain (GLS) of all the different strain methodologies that we've had has become the one that people use,” said Michael McElroy, solutions marketing senior manager at Canon Medical Systems USA. “We finally have a standard of strain.”
Strain imaging provides an earlier prediction of cardiac issues before the ejection fraction (EF) changes. By the time the EF changes, that’s the indicator of major issues with myocardial function.
Last year, Canon released its Auto EF with GLS tool for its Aplio a-series and i-series ultrasound systems. By hitting one button, this tool automatically provides the clinician with the EF and GLS number.
Finding the right views in each echo exam and EF and GLS is also a cumbersome process. This task typically takes stenographers a couple of minutes to complete, but they can get those numbers in a couple of seconds with this tool.
DiA also launched a new tool for this called LVivo Seamless. It automatically obtains optimal views and cardiac measurements for every cardiac ultrasound exam in the echo lab.
There are usually between 50 and 60 views in a standard echo exam and this tool pre-selects the optimal views for the calculation of EF and GLS.
An area that GLS is showing promise in is chemotherapy. Many chemotherapy agents can damage the heart muscle, so GLS is being used with the highest sensitivity to assess any potential damage.
“The tightrope that the oncologist is walking is whether they can use the agent and not put the patient in unrecoverable heart failure because of the myocardial toxicity of the agent,” said McElroy.
GLS strain imaging provides an earlier indication of chemotherapy toxicity before the EF changes. It’s thought that once the EF goes down, the damage is permanent, but if the clinician spots the change in strain GLS early on, they can adjust the chemotherapy regimen and preserve the EF and have good oncological and cardiological outcomes.
Despite its benefits, adoption remains slow. According to McElroy, the routine use of strain imaging among cardiologists is within the 20 to 30 percent range, its use in doctor’s offices is about 10 percent and at the university level it’s upwards of 100 percent.
Structural heart disease
The global structural heart devices market is projected to reach $13 billion in 2027, according to a new Transparency Market Research report. New procedures for aortic stenosis and mitral regulation are driving this trend, as well as the rising geriatric population.
“Considering the growing number of structural heart procedures, innovations in this area are game changers,” said Elizabeth Oakes, senior director, clinical strategy at Siemens Healthineers.
The company recently launched a product that has the potential to greatly improve procedural efficiency in this area. The latest ACUSON SC2000 PRIME 6.0 ultrasound system features 4D Volume Intracardiac Echocardiography (ICE) capability with the ACUSON AcuNav Volume ICE catheter.
This is currently the only commercially available 4D Volume ICE catheter on the market as of February 2021. It provides more real-time information in one view to accurately navigate, guide and measure with multiplanar reconstruction planes (MPRs).
This technology also has the potential to reduce the need for general anesthesia as well as scheduling effort, staffing needs, procedural time, and cost compared to transesophageal echocardiogram (TEE)-guided procedures.
A 2017 study published in JACC: Cardiovascular Interventions found that left atrial appendage closure procedures performed with ICE led to 57 percent time savings per case compared to TEE.
4D Volume ICE allows physicians to offer treatment to patients that would otherwise have no options for structural heart disease procedures. These patients cannot undergo TEE or general anesthesia, or any procedure that requires optimal imaging of the tricuspid valve.
Philips is also making headway in this field with its new automated tools for mitral valve and left atrial appendage measurement, Auto MVA and LAA solution, and its new visualization tools, TrueVue Glass. These tools are for use with the company’s EPIQ CVx ultrasound system.
“[Our new tools] provide a unique way of analyzing the heart structure and function with transparency,” said Philips’ Goncalves.
During interventional echo procedures, the system visualizes the morphology of the left atrial appendage (LAA) and automatically measures the ostium. It also automatically assesses the mitral valve and obtains multiple measurements and functional data.
“2020 was a year of innovation with exciting new features for assessment of structural heart disease and procedure guidance,” said Goncalves. “3D techniques have been evolving to provide better visualization, efficient quantification and safe guidance for the challenging structural heart disease procedures.”