FDA warns women about mammography 'alternative'
by
Brendon Nafziger, DOTmed News Associate Editor | June 03, 2011
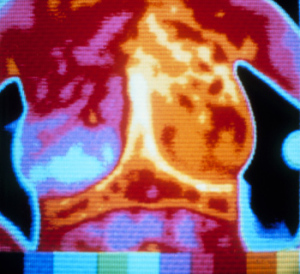
A thermography chest
image. (Credit: FDA)
The Food and Drug Administration has warned women to be wary of an infrared-imaging technique some websites tout as a "radiation-free" alternative to mammography.
The agency told consumers Thursday that a technique that uses infrared imaging to measure heat and blood flow, called thermography, should not be used in place of mammography for cancer screening or diagnosis.
The agency also said this year alone it had already sent a trio of warning letters to those whom the agency said promoted the "inappropriate use" of the technology. Recipients of the letters include a manufacturer of a thermography device, a natural health website and a California breast imaging center, the agency said.
The agency said some thermography promoters claimed thermography could diagnose breast cancer by itself or even catch pre-cancerous growths years before mammography would discover them. Neither claim is supported by scientific evidence, the FDA said.
"While there is plenty of evidence that mammography is effective in breast cancer detection, there is simply no evidence that thermography can take its place," Dr. Helen Barr, director of the Division of Mammography Quality and Radiation Programs in the FDA's Center for Devices and Radiological Health, said in a statement.
Thermography uses an infrared camera to measure differences in temperature, producing an infrared image familiar to anyone who has seen the movie "Predator." The FDA has cleared thermography devices for use as an adjunct to other technologies but not for use by itself to diagnose or screen for cancer.
Writing about the misleading promotional claims surrounding thermography on the Science-Based Medicine blog last year, Dr. David Gorski, a cancer surgeon, said the idea behind thermography is that potentially dangerous tumors need to be fed by new blood vessels, which result in increased blood flow and thus, increased heat. Also, breast cancers have increased metabolic activity and inflammation, which could also lead to higher heat.
But Gorski and other imaging and cancer experts say the studies so far done on the technology since the first thermography scan in 1956 are not convincing.
"It's unreliable, and it doesn't provide much in the way of anatomic information that allows a better localization of the breast cancers it does find," Gorski wrote last year.
Both the American College of Radiology and the Society of Breast Imaging have issued statements saying they don't support using the device even as an adjunct to mammography, saying that the research on the technology -- mostly decades old -- hasn't shown it to be effective.
"The position of the American College of Radiology is that thermography has not been demonstrated to have value as a screening, diagnostic or adjunctive imaging tool," the group said in a statement this week. "We are pleased that the FDA has taken this step to clarify its view on thermography."
In a message posted to its website, SBI said most research on thermogaphy has not been done on women who would make up a screening population, nor have researchers compared the modality to mammography with technologies proven to increase diagnostic accuracy, such as ultrasound, breast MRI or nuclear medicine.
|
|
|
You Must Be Logged In To Post A Comment
|

Jose Morillo
A SAFE ALTERNATIVE IS URGENT
June 09, 2011 03:39
I had serviced these machines, I has place my hand under the compressor device and test in my hand the pressure women support on her bust.. It's like a teenager step on your hand. Radiation itself mean a big problem due each bust receive two shoots each year. If termal imaging can solve the problem, a comparative study can probe it in few years. IT MUST BE INVESTIGATE!. High resolution ecógraphy, MRI, blood testing, etc. No option must be subestimated! perhaps to blend two or more of those exams and correlationate results can aid to avoid or reduce the needed of mammographies.
I think is cheaper than develope a new tecnology and faster try to apply well known technologies than wait for a new one.
to rate and post a comment