by
Heather Mayer, DOTmed News Reporter | July 22, 2010
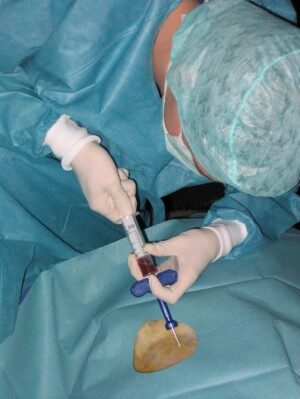
Bone marrow transplants
could carry less
risk.
A new technique that depletes certain immune cells could improve the treatment of leukemia relapse after bone marrow transplants, resulting in an effective therapy for patients with resistant cancers, according to research published today in Science Translational Medicine.
Patients who undergo bone marrow transplants often develop graft-versus-host disease, in which the transplanted, or grafted, immune cells attack the host tissues. While this condition can help fight cancer because it attacks cancerous tissue, it can also increase a patient's risk of dying in remission when more healthy tissue is destroyed.
Ordinarily, bone marrow transplants use a phenomenon called allo-immunity to destroy foreign elements, explained researcher Jose Cohen in an e-mail to DOTmed News. But in many cases, immune tolerance is established, thought to be related to regulatory T-cells.




Ad Statistics
Times Displayed: 45178
Times Visited: 1385 Keep biomedical devices ready to go, so care teams can be ready to care for patients. GE HealthCare’s ReadySee™ helps overcome frustrations due to lack of network and device visibility, manual troubleshooting, and downtime.
What the French researchers, led by Dr. Sebastien Maury, found was that depleting these regulatory T-cells in donor tissue improves the graft-versus-host disease effect after bone marrow transplants and consequently the anti-tumor effect.
"The risk for the patient before our cell therapy is to die from relapse of hematolocical cancer," said Cohen. "The risk for the patient after our cell therapy is to develop a graft-versus-host disease, which is a too strong immune response of the donor against the recipient."
Cohen pointed out that the researchers only included patients with very low risk of developing graft-versus-host-disease.
The study included 17 leukemia or lymphoma patients who underwent bone marrow transplants but whose cancers returned. In order to treat the relapse, the researchers eliminated the population of regulatory T-cells in new tissue collected from the same donors and then transplanted this tissue into the patients, according to the report. The depletion of these T-cells increased the graft-versus-host disease effect in six patients; the transplanted donor cells killed more cancer cells more effectively. Three patients are now cancer-free.
"This study is a proof of concept that demonstrated that regulatory T-cell manipulation can have therapeutic effects in humans," said Cohen. "It opens the way to the application of regulatory T-cell manipulation in various fields of medicine where the immune system needs to be tolerized in autoimmune diseases or un-tolerized in cancer."
Moving forward, the researchers plan to refine the technique "as an effective way to cure patients with very resistant cancers with an improved form of bone marrow transplants, bringing new hope to patients," said Cohen.

