by
Lauren Dubinsky, Senior Reporter | October 07, 2016
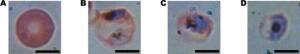
Four cells under a microscope in different
stages of malaria infection
Courtesy of Adam Wax
In developing countries, malaria is a major issue and there aren't enough well-trained field workers and functioning microscopes to diagnose it. To solve that, researchers at Duke University have developed a technique that uses computer "deep learning" and light-based, holographic scans to diagnose the disease.
In 2015, there were about 214 million malaria cases and an estimated 438,000 malaria deaths, according to the World Health Organization. Western countries are able to accurately diagnose malaria, but the tests they use are expensive.
In a new study published in the journal
PLOS ONE, the Duke researchers used the technique to identify cells infected with malaria from a simple, untouched blood sample. The results may become the basis for a fast and reliable test that anyone can administer.




Ad Statistics
Times Displayed: 2436
Times Visited: 4 Stay up to date with the latest training to fix, troubleshoot, and maintain your critical care devices. GE HealthCare offers multiple training formats to empower teams and expand knowledge, saving you time and money.
"With this technique, the path is there to be able to process thousands of cells per minute," Adam Wax, professor of biomedical engineering at Duke, said in a statement. "That's a huge improvement to the 40 minutes it currently takes a field technician to stain, prepare and read a slide to personally look for infection."
The technique is based on a technology called quantitative phase spectroscopy. A laser sweeps through the visible spectrum of light and sensors capture how each light frequency interacts with the blood sample.
That data is used to generate a holographic image that reveals valuable information that can be used to diagnose the patient. The researchers identified 23 parameters that can be used to diagnose malaria.
As the disease progresses, the amount of red blood cells decreases, lose hemoglobin, and become deformed. That has an effect on cell volume, perimeter, shape, and center of mass, which can be detected with the technique.
But since none of the parameters were more than 90 percent reliable on their own, the researchers decided to use all of them. Over 20 million cases per year could be missed if a test is only 90 percent reliable.
The researchers leveraged a deep learning program to make the technique more accurate. They fed data on over 1,000 healthy and diseased cells into a computer, and the program determined the measurements that more accurately distinguished the cells.
When they tested it with hundreds of cells, it was able to identify malaria 97 to 100 percent of the time. They believe that percentage will be higher once more cells are used to train the program.
Wax and the other researchers are looking to translate the technique into a diagnostic device. They started a company called M2 Photonics Innovations, and have received funding to also investigate its usefulness for identifying cancer cells in blood samples.
Back to HCB News
