by
Lauren Dubinsky, Senior Reporter | November 29, 2017
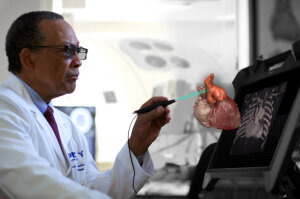
New version supports ultrasound
and C-arm images
CHICAGO — Stanford University Medical Center presented a scientific poster at the RSNA annual meeting on Sunday that explored medical applications for EchoPixel’s new True 3D virtual reality software.
“I don’t see why a doctor should use a 2-D image in 2017,” Sergio Aguirre, CEO of EchoPixel, told HCB News.
True 3-D leverages DICOM imaging data to generate life-sized holograms of organs, blood vessels and other structures. For surgical planning, physicians and surgeons can rotate, resize, dissect and make incisions to the patient-specific holograms.




Ad Statistics
Times Displayed: 2436
Times Visited: 4 Stay up to date with the latest training to fix, troubleshoot, and maintain your critical care devices. GE HealthCare offers multiple training formats to empower teams and expand knowledge, saving you time and money.
The software received FDA approval in 2015 to support CT and MR images. EchoPixel released version 1.6.2 in March 2016, which supports ultrasound with Doppler and C-arm fluoroscopy images and features a new reporting structure.
Stanford deployed True 3D in its operating room, to be used for intraoperative imaging consultation, and found that it was effective at conveying patient-specific information to the surgical team. They also used it for complex pulmonary artery reconstruction, sternotomy planning before minimally-invasive valve replacement surgery and separating conjoined twins.
According to the findings, True 3D is also a helpful tool for radiologists when anatomy is variable or unexpected. It comes with a suite of processing tools including a programmable transfer function, color map, interactive cropping tool and 4-D-cine to effectively examine the interior structures of the heart.
Aguirre cautioned that True 3D is not meant to replace 3-D printing, but instead to complement it. Stanford proposed that True 3D can be used first to explore the data set and plan the optimal cut plane and segmentations, and the results can be transferred electronically for 3-D printing.
“A lot of times surgeons will still want to feel something in their hand and we don’t do that," said Aguirre.
