by
John R. Fischer, Senior Reporter | February 22, 2019
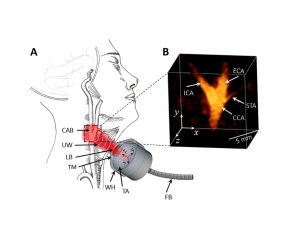
vMSOT applies spectroscopy to
investigate tissue at the molecular
level to accurately assess the risk
of cardiovascular disease
A new study is touting the use of a noninvasive technique for imaging the carotid artery to accurately assess the risk of cardiovascular disease, compared to traditional modalities.
Known as volumetric multi-spectral optoacoustic tomography (vMSOT), the approach encompasses the use of a handheld device that applies spectroscopy to investigate tissue at the molecular level while moved against the neck.
"At present, carotid artery disease is mainly assessed with duplex ultrasound, computed tomography and magnetic resonance imaging," study senior author Dr. Daniel Razansky, director of the functional and molecular imaging lab at the University of Zurich and the Swiss Federal Institute of Technology, told HCB News. "These modalities can provide anatomical visualization of the carotid artery. However, rapid characterization of tissue function and molecular composition is limited with these modalities, which commonly results in poor diagnostic accuracy and ineffective treatments."




Ad Statistics
Times Displayed: 2130
Times Visited: 4 Stay up to date with the latest training to fix, troubleshoot, and maintain your critical care devices. GE HealthCare offers multiple training formats to empower teams and expand knowledge, saving you time and money.
Though capable of determining the extent of narrowing in the carotid arteries, traditional modalities such as ultrasound, CT and MR are limited in their ability to determine the composition of plaques within the arteries, the knowledge of which can indicate their vulnerability to rupture. The occurrence of such an event can lead to life-threatening strokes.
The practice of vMSOT provides data about the artery that is not obtainable with other approaches, and can evaluate other disease-related biomarkers early enough for determining better treatment options, such as lipids and pigment melanin.
Researchers applied vMSOT imaging to 16 healthy patients and compared the results to ones assessed with ultrasound. They found the vMSOT methods to be less prone to motion-related, image-blurring artifacts, compared to ultrasound, while noninvasively and instantly assessing the entire bifurcation area of the carotid artery in three dimensions.
The method also holds potential for label-free identification and assessment of clinically-relevant biomarkers of carotid artery disease, aiding in its early and accurate diagnosis for timely treatment, planning and monitoring, according to Rasansky, who adds that it could be combined at some point in the future with ultrasound to provide a more comprehensive description of the carotid artery.
"Several efforts are underway to apply it to noninvasive detection of breast malignancies, lymph node metastases, diagnostics and staging of inflammation and cardiovascular diseases, characterization of skin lesions, to name a few examples," he said. "Vast efforts need to be invested into making the technology more robust and affordable, tailor it for specific applications, develop approaches for accurate image reconstruction, interpretation and quantification."
The findings were published in the journal,
Radiology.

