by
John R. Fischer, Senior Reporter | August 27, 2019
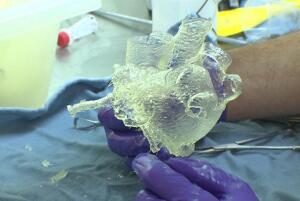
VA Puget Sound Health Care System
and UW Medicine are developing new
3-D printing approaches to address heart
problems
A Veteran Affairs healthcare system has teamed up with the University of Washington School of Medicine to develop new approaches in 3D printing for the diagnosis and treatment of complex heart conditions.
The VA Puget Sound Health Care System and UW Medicine have agreed to share their 3D printing technology, materials, software and staff with one another to establish new protocols for better planning procedures by providing greater clarity to cardiologists for visualizing complex anatomies unique to each patient. The products are expected to open up access and outcomes for new minimally-invasive treatments.
“Our collaboration is expected to impact a wide variety of patients, including those with resectable tumors such as renal or prostate malignancies, those with complex pelvic fractures, and those undergoing spinal surgeries,” Dr. Beth Ripley, a VA Puget Sound radiologist and chair of the VA's advisory panel on 3D printing, and a UW assistant professor of radiology, told HCB News. “Patients requiring vascular treatments such as aortic aneurysm repair are also a natural extension from our existing work with structural heart disease.”



Ad Statistics
Times Displayed: 2147
Times Visited: 10 Fast-moving cardiac structures have a big impact on imaging. Fujifilm’s SCENARIA View premium performance CT brings solutions to address motion in Coronary CTA while delivering unique dose saving and workflow increasing benefits.
Ripley says more cases that can potentially benefit from 3D printed models are expected in the changing healthcare environment. A recent FDA decision last week to approve a catheter-based approach to aortic valve replacement devices in low-risk patients is one example, as such patients are often directed to undergo surgery.
Both early adopters of the technology, VA Puget Sound and UW Medicine have conducted a number of research endeavors in the field of 3D printing that have led to important insights. For instance, the VHA 3D printing network has used its research to develop a number of models, from those of kidneys for pre-surgical planning for veterans with renal cancer to specialized foot orthotics to help avoid amputations for veterans with type 2 diabetes.
The UW School of Medicine, meanwhile, brings to the table its nationally recognized 3D printing lab that has produced more than 100 patient-specific models to guide the decisions of cardiologists and surgeons.
The two expect their work to support future research, development and scalability of 3D printing applications for advanced treatment approaches for complex conditions, such as mitral valve disease, as well as help clinicians determine how to best approach particular structures, and which catheters and replacements to use in operations. They also expect it to help direct healthcare in the direction of bio-printing.
While the VA project to bio-print living, vascularized bone is not currently part of this partnership, the agreement opens the door wide for a future collaboration,” said Ripley, adding that “a key partner in the bio-printed bone effort, head and neck surgeon Dr. Jeffrey Houlton, takes care of patients at both UW Medicine and the VA, so this would be a natural fit.”

