by
John R. Fischer, Senior Reporter | April 09, 2021
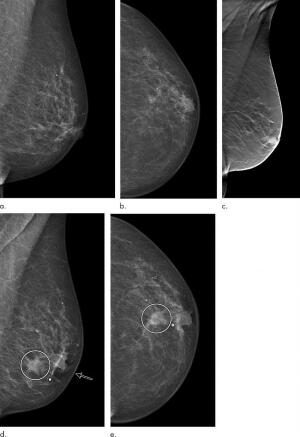
Digital breast tomosynthesis may help reduce the rate of interval cancers in patients better than digital mammography
Screening with digital breast tomosynthesis may help reduce interval breast cancer rates.
That’s what a new study out of Skåne University Hospital and Lund University in Sweden says, adding to growing evidence that DBT holds significant advantages over mammography.
Interval cancers arise in between screenings and are considered more aggressive than screen-detected cancers. The interval cancer rate among nearly 15,000 women screened in the study with DBT and DM was 1.6 per 1,000, compared to 2.8 per 1000 out of 26,000 who only received DM. Interval cancers found generally had unfavorable characteristics.




Ad Statistics
Times Displayed: 1552
Times Visited: 2 Stay up to date with the latest training to fix, troubleshoot, and maintain your critical care devices. GE HealthCare offers multiple training formats to empower teams and expand knowledge, saving you time and money.
"DBT has in several trials been shown to have a higher breast cancer detection rate in screening compared to digital mammography. The higher cancer detection rate with DBT might translate into lower interval cancer rates, and this is what has been shown in our trial," lead author Dr. Kristin Johnson, a radiology resident at Skåne University Hospital and Ph.D. student at Lund University, told HCB News.
The decrease in interval cancers may be due to the heightened sensitivity of DBT over DM, according to the authors, which gives it the potential to better detect rapidly growing cancers with poorer prognosis. This could lower breast cancer mortality and may even pave the way for DBT to eventually replace DM in the future, according to Johnson.
She stresses, however, that other trials have not seen significant reductions in interval cancer rates in DBT screening when compared to mammography, and that interval cancer rates are not the only measure that define the effectiveness of DBT. "Our study is, so far, the only study which has shown reduced interval cancer rates with DBT compared to DM and more studies are needed to confirm the results."
Johnson and her colleagues are working on a cost-benefit analysis of the Breast Tomosynthesis Screening Trial, where the interval cancer rates came from, for their study. They are also evaluating the trial for false positive recalls.
The findings were published in
Radiology.

