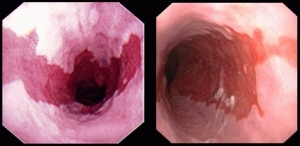
When patients with
Barrett's esophagus develop
esophageal cancer, the
cancer is usually deadly
A procedure that uses heat generated by radio waves to treat Barrett's esophagus, a condition caused by acid reflux, is proving to be highly successful.
The current trial by device manufacturer, Barrx Medical, published in the May 28 issue of The New England Journal of Medicine, confirms data Barrx presented at a gastroenterology conference last May. (See DM 6059).
This is the first multicenter trial using the procedure. Treating Barrett's is important, since the risk of progressing from Barrett's to esophageal cancer is approximately 1 percent for those with low-grade dysplasia and 6 percent for those with high-grade disease.



Ad Statistics
Times Displayed: 79569
Times Visited: 2807 Ampronix, a Top Master Distributor for Sony Medical, provides Sales, Service & Exchanges for Sony Surgical Displays, Printers, & More. Rely on Us for Expert Support Tailored to Your Needs. Email info@ampronix.com or Call 949-273-8000 for Premier Pricing.
And when patients with Barrett's esophagus develop esophageal cancer, the cancer is usually deadly, says Steven A. Edmundowicz, M.D., lead investigator at the study site at Washington University School of Medicine in St. Louis. He says that fewer than 15 percent of patients with esophageal adenocarcinoma survive for five years.
Doctors conducting the study treated a total of 127 patients at 19 sites, using endoscopes to diagnose the disease and then to deliver radiofrequency ablation to the abnormal lining of the esophagus. The technique heats the abnormal tissue to destroy it while leaving the deeper layers of the esophagus undamaged.
Led by Nicholas J. Shaheen, M.D., at the University of North Carolina at Chapel Hill, the investigators at the various study sites randomly selected patients to either receive radiofrequency ablation or to undergo a sham procedure in which endoscopes were inserted through the mouth and the lining of the esophagus was examined, but no radio waves were delivered.
Two patients received the actual treatment for every one who got a sham procedure. Those who received the ablation treatment could get up to four treatments during the 12 months of the study. Following the study period, those who had not received ablation therapy were given the option of getting the treatment.
High Success Rate
In the patients who had the treatment, dysplasia disappeared in approximately 90 percent of patients with low-grade disease and in more than 80 percent of those with high-grade disease compared to about 23 percent of the low-grade patients and 19 percent of the high-grade patients who had sham procedures.
In 78 percent of treated patients, not only did dysplasia disappear, but all the abnormal intestinal-type cells were eliminated as well.
"During the 12-month study period, we detected fewer cancers in the ablation group than in the control group," says Edmundowicz, a professor of medicine in the Division of Gastroenterology. "But because cancers occurred in a total of only five study patients, the numbers are not as powerful regarding cancer as they are regarding eradication of Barrett's esophagus."
In Barrett's esophagus, part of the lining of the esophagus is replaced with cells that resemble intestinal cells. As the condition progresses, these cells become increasingly disordered. Long-standing acid reflux disease is common in those who develop Barrett's esophagus, which affects about 1 percent of adults in the United States.
Source: Washington University in St. Louis

