by
John R. Fischer, Senior Reporter | September 23, 2020
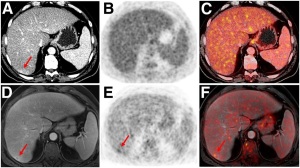
PET/MR improves lesion detection, reduces radiation exposure and is just as effective as PET/CT in staging cancer
PET/MR facilitates cancer staging just as well as PET/CT, improves detection of lesions in select cancers and significantly reduces overall radiation exposure.
That’s according to a single-center observational study of more than 1,000 oncological exams studied by researchers in Germany.
"Due to the higher soft tissue contrast, PET/MR improves lesion detection and reduces the need for additional examinations in comparison to PET/CT," said Dr. Benedikt Schaarschmidt, professor and radiologist at the University Hospital Essen, in a statement. "Especially in younger patients who need repeated diagnostic procedures, our data advocate the use of PET/MR due to the markedly reduced radiation exposure of PET/MR when compared to PET/CT."



Ad Statistics
Times Displayed: 345431
Times Visited: 21060 MIT labs, experts in Multi-Vendor component level repair of: MRI Coils, RF amplifiers, Gradient Amplifiers Contrast Media Injectors. System repairs, sub-assembly repairs, component level repairs, refurbish/calibrate. info@mitlabsusa.com/+1 (305) 470-8013
While recommended by various oncologic imaging guidelines due to its sensitivity and high-resolution morphologic imaging, PET/CT does not have as high soft-tissue contrast as PET/MR and can expose patients to a high amount of radiation. The lack of clinical studies with relevant sample sizes for PET/MR has led to a scarcity of clinical evidence that demonstrates its efficiency, and is the reason why it is not as widely used for oncologic imaging as PET/CT is, according to the authors.
The researchers performed 1,003 whole-body PET/MR exams on 918 patients at a single center and compared the scans to images from whole-body PET/CT exams of the same patients. Among the oncological indications were lung cancer, gastrointestinal cancer or neuroendocrine cancer, gynecologic or breast cancer, prostate cancer, lymphoma, melanoma, head and neck cancer, cancer of unknown primary, and malignant bone disease.
Board-certified nuclear medicine physicians and radiologists assessed the exams for additional findings on PET/MR that were missing on PET/CT and probable diagnoses. They also searched for additional indeterminate findings on PET/MR that require additional exams or follow-ups; classification of indeterminate findings on PET/CT by PET/MR; and missed findings on PET/MR compared to PET/CT. Effective dose of both modalities was also examined.
The study showed additional information on PET/MR was reported for 26.3% of exams, compared to PET/CT. Of these, additional malignant findings were detected in 5.3%, changing TNM staging in 2.9% due to PET/MR. Definite lesion classification of indeterminate PET/CT findings was possible in 11.1% with PET/MR, while 2.9% of lesions detected on PET/CT were not visible on PET/MR. Malignant lesions were missed in 1.2% on PET/MR, changing TNM staging in 0.5%, and the estimated mean effective dose for whole-body PET/CT was 17.6 ± 8.7 mSv, compared to 3.6 ± 1.4 mSv for PET/MR. This translates to a potential dose reduction of 79.6%.
The improvement in lesion detection in select cancers potentially enables fast, efficient local and whole-body staging in one step, while significant reductions in overall radiation exposure for PET/MR compared to PET/CT greatly benefits pediatric and adolescent patients, according to the authors.
"Hybrid imaging examinations are now part of complex diagnostic algorithms in multiple cancer types,” said Schaarschmidt. “Based on our data, PET/MR could be an important adjunct to PET/CT by providing diagnostic advantages and improving diagnostic algorithms in numerous cancers at the same time. Furthermore, the markedly reduced radiation exposure of PET/MR could lead to a more frequent use of this examination in oncological patients, most notably for treatment monitoring."
The findings were published in
The Journal of Nuclear Medicine.

