by
John R. Fischer, Senior Reporter | October 15, 2020
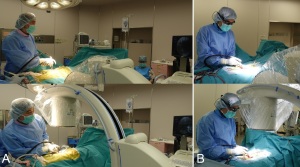
A new eyeglass-attached display device enables surgeons to directly view fluoroscopic images
Two Japanese surgeon-researchers have developed an eyeglass capable of displaying fluoroscopic images for directly guiding surgeons during operations.
The solution is meant to allow the surgeon to see both the surgical field and information displayed on monitors simultaneously, without having to look across the operating room to a video monitor. The developers, Dr. Keitaro Matsukawa, M.D., Ph.D., and Dr. Yoshiyuki Yato, M.D., Ph.D., claim that this slightly shortens the length of surgery, reduces risk of error and decreases radiation exposure.
"The device allows users to focus on their critical tasks by improving ergonomics during procedures," Matsukawa told HCB News. "I think this is a powerful device that present a variety of information to the wearer's eyes to provide smooth and efficient medical care."




Ad Statistics
Times Displayed: 1552
Times Visited: 2 Stay up to date with the latest training to fix, troubleshoot, and maintain your critical care devices. GE HealthCare offers multiple training formats to empower teams and expand knowledge, saving you time and money.
Navigation systems like monitors are not always in the most convenient place in the operating room, with surgeons having to look up and turn their heads during procedures to view their progress, especially during fluoroscopic operations where the monitor is several feet away from the operating table. The constant movement can distract the surgeon, leading to longer procedure times, technical difficulties and potential errors.
The authors tested the efficiency of their device in a pilot randomized study of 20 patients who underwent posterior lumbar interbody fusion at the L5-S1 spinal level. They hypothesized that wearing a device that displays fluoroscopic images within the surgeon’s visual field during insertion and attachment of spinal instrumentation would improve the safety of the minimally invasive operation.
All surgeries were performed by the same surgeon, who used the percutaneous pedicle screw technique in each case. Ten cases involved the surgeon wearing glasses with an attached device (picoLinker device, Westunitis) which wirelessly displayed real-time fluoroscopic images, while the other 10 involved the surgeon wearing no display device and relying on a fluoroscopy monitor positioned elsewhere in the OR. The authors examined the number of times the surgeon’s head turned to consult the fluoroscopic video display and then compared the duration of operations and length of time the patient and surgeon were exposed to radiation emitted by the fluoroscope.
Operations where the surgeon wore the device involved less head turning (means ± standard deviations: 0.1 ± 0.31 vs. 82.4 ± 32.5 times; p < 0.001) and were shorter in duration (100.2 ± 10.4 vs. 105.5 ± 14.6 minutes). Length of radiation exposure was also shorter (38.6 ± 6.6 vs. 41.8 ± 16.1 seconds) when the device was worn. Only one intraoperative complication, a screw perforation, occurred when the surgeon was not wearing the display device.
Matsukawa and Yato say that to their knowledge that this is the first study on the feasibility of using a wearable display device for fluoroscopically guided, minimally invasive, spinal instrumentation surgery.
"We consider it useful in all procedures where you are forced to take your eyes off from operative fields to check various monitors, particularly in surgeries that use navigation and intraoperative fluoroscopy and ultrasound devices," said Matasukawa. "In the future, we believe that the system can be applied to telemedicine by using audio and recording functions."
The two are attempting to apply the solution in various surgeries, including intraoperative navigation.
There are no plans to pursue any regulatory approval at this time.
The findings were published in the
Journal of Neurosurgery: Spine.
