by
John R. Fischer, Senior Reporter | August 25, 2023
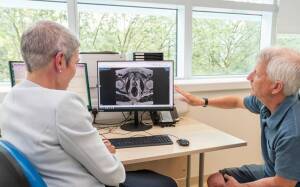
MR imaging and PSA density testing can catch significant cases of prostate cancer that a blood test alone missed.
In the REIMAGINE Study, a multicenter, prospective trial assessing the need for more NHS tests to screen for prostate cancer, British researchers say that applying MR imaging and PSA density testing together lowers the risk of missing cancers compared to using a blood test alone.
Using both tools may also reduce overdiagnosis, a common occurrence with PSA and digital rectal exams, say the authors, from University College London, University College London Hospital, and King’s College London, whose study saw less than 1% of participants overdiagnosed.
Among 303 men between 50 and 75 who underwent MR scans and PSA tests, 48 (16%) received a positive screening that indicated potential cancer despite having a median PSA density result of 1.2 ng/ml. Of these 48, 32 showed levels below the current screening benchmark of 3ng/ml, meaning that with a blood test alone, they would not have been referred for additional testing.



Ad Statistics
Times Displayed: 344592
Times Visited: 21056 MIT labs, experts in Multi-Vendor component level repair of: MRI Coils, RF amplifiers, Gradient Amplifiers Contrast Media Injectors. System repairs, sub-assembly repairs, component level repairs, refurbish/calibrate. info@mitlabsusa.com/+1 (305) 470-8013
Following this, 29 (9.6%) were diagnosed with cancer that required treatment, including 15 with serious cases who had a PSA of less than 3 ng/ml, while three (1%) had low-risk cancer that did not require interventions.
“The thought that over half the men with clinically significant cancer had a PSA less than 3 ng/ml and would have been reassured that they didn’t have cancer by a PSA test alone is a sobering one and reiterates the need to consider a new approach to prostate cancer screening,” said professor Caroline Moore, UCL surgical and interventional science and consultant surgeon at UCLH, chief investigator of the study, and NIHR Research Professor, in a statement.
Clinicians began using MR to screen for prostate cancer a few years ago, and have since seen one in four men spared from unnecessary and invasive biopsies that can lead to complications, say the researchers.
The findings here provide insights for the formation of a national screening program for prostate cancer in the U.K., but further studies with larger groups are necessary to validate the use of this approach.
The researchers are already planning a follow-up, the LIMIT trial, and say that any future studies should incorporate ways of recruiting more Black patients to undergo prostate cancer screenings, as one in four will develop prostate cancer during their lifetime, which is double that of men from other ethnic backgrounds. Despite this, Black men are five times less likely to sign up for the REIMAGINE Study.
To actively recruit more, the group will use mobile "scan in a van" initiatives to visit communities that are less likely to come forward for testing.
“It will be crucial that any national screening program include strategies to reach black men and encourage more of them to come forward for testing,” said Saran Green, an author of the study from King’s College London.
The findings were published in
BMJ Oncology.

