by
Barbara Kram, Editor | March 19, 2008
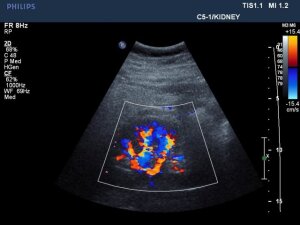
Kidney bloodflow visualized
by Philips' C5-1 ultrasound
probe technology
The rising prevalence of obesity in the U.S. and globally has challenged ultrasound systems to penetrate fatty tissue more effectively to obtain diagnostic views. Up to half of all abdominal ultrasound exams are conducted on large patients.
Fortunately, this technical challenge coincides with some cutting-edge R&D from Philips to develop a new type of crystal that can penetrate fatty tissue to reveal pathology beneath.
It's helpful to understand that ultrasound transducers use a piezoelectric material to deliver the ultrasound energy to the scanned tissue and convert resulting echoes into electrical signals. However, today's widely used crystal type, known as PZT, has its limitations, achieving only about 70% efficiency. A better type of piezocrystal has been discovered but has proven difficult to grow. Philips engineers have been working on this problem and made recent breakthroughs in both crystal growth and crystal properties. The result is a crystal technology they call PureWave, which are purer and more uniform crystals that can transfer energy with greater precision and efficiency. This material supports improved penetration in difficult patients, and excellent detail of the heart's fine structures. The technology can also be used in imaging other organs.



Ad Statistics
Times Displayed: 45539
Times Visited: 1299 Ampronix, a Top Master Distributor for Sony Medical, provides Sales, Service & Exchanges for Sony Surgical Displays, Printers, & More. Rely on Us for Expert Support Tailored to Your Needs. Email info@ampronix.com or Call 949-273-8000 for Premier Pricing.
The Philips technologies that tap this innovation include the iU22 ultrasound system with the C5-1 transducer. Features of the system include tissue aberration correction and a functionality known as coded beamforming to reduce image degradation.
The chief challenge with obese patients is that their livers and other abdominal organs are more than 5 centimeters deep; the prevalence of fat and fatty livers are difficult to characterize. Using conventional ultrasound technology, it takes longer to perform the imaging study on difficult patients and they are ergonomically difficult for sonographers to manipulate. The image itself is degraded by changes in sound wave transmission through fat so the image loses resolution.
"We are seeing in our practice that obesity is increasing and there is also a rise in fatty livers, which is related to alcohol. However ultrasound has difficulty penetrating fat because it acts like fog to ultrasound," explained Simon Elliott, MD, radiologist at the Freeman Hospital in Newcastle, UK, who first began testing the device last year. "It is just like shining a torch [flashlight] into fog. You often cannot see organs and if you can see them it may still be difficult to make a diagnosis."

