by
John R. Fischer, Senior Reporter | November 20, 2019
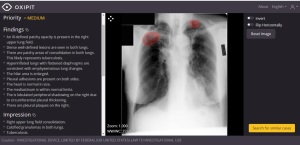
A new study says AI CAD software like Oxipit
Chest AI imaging suite can reduce bias in
radiology reports
A new study is claiming that AI-powered CAD software can reduce bias in radiology reports.
The research, conducted by the Centre for Advanced Research in Imaging, Neuroscience and Genomics (CARING), found that such technology eliminates hedging and defensive reporting statements, thereby producing more actionable diagnostic descriptions. Its claim is based on an assessment of Oxipit Chest AI imaging suite, a fully automatic computer-aided diagnosis (CAD) platform designed by software company Oxipit.
"Sometimes radiologists might be fairly confident that there is no pathology in the analyzed case, but they choose to include inconclusive vague diagnosis statements to hedge against potential mistakes or legal threats," Oxipit’s chief medical officer Dr. Naglis Ramanauskas, told HCB News. "This hedging can potentially result in inconclusive reports which might cause unnecessary examinations, such as further CT scans, or unnecessary treatment applications such as prescribing antibiotics for a misdiagnosed pneumonia."




Ad Statistics
Times Displayed: 2130
Times Visited: 4 Stay up to date with the latest training to fix, troubleshoot, and maintain your critical care devices. GE HealthCare offers multiple training formats to empower teams and expand knowledge, saving you time and money.
Inconclusive reports shift decisions around treatment back to the referring physician, who is left on his or her own with no aid for prescribing a course of action.
Oxipit ChestEye AI imaging suite supports 75 radiological findings, covering more than 90 percent of radiological cases presented to radiologists daily. It generates a standardized preliminary text report of all radiologically relevant information present in a chest X-ray. These features help to speed up case descriptions, while reducing the risk of overlooked secondary findings.
Researchers applied the solution to 297 retrospective chest X-ray images, and compared its reports to those written up by a radiologist. A final comparison and diagnosis validation was completed by a radiologist with nine years of clinical experience.
The solution’s reports were accurate to those of radiologists 80 percent of the time. It also generated ones that were five percent more accurate in analyzed patient cases. Further supporting its efficiency are internal platform trials that found it shaved off 30 percent of time required per patient case and reduced the rate of error by up to 50 percent.
But Ramanauskas says that any report from the solution must be backed up by the radiologist's expert opinion. "An X-ray report is not a simple description of image. The reports should include expertise-based judgment. The radiologist could put himself or herself in the shoes of the referring clinician — 'does the report I produce provide actionable insights toward further patient treatment? Does my report aid the decision-making? Would I feel less uncertain toward treatment decisions after reading the report?'"
The solution
is CE marked and available for use in 32 European nations.

